How long does a Hysteroscopy take
Type of Hysteroscopy:
Diagnostic types, which involves only visualization and examination of the uterine cavity. How long does a Hysteroscopy take, it is typically quicker than operative works where surgical interventions may be performed.
Complexity of the Case:
How long does a Hysteroscopy take, it can affect the procedure’s duration. For example, removing multiple polyps or fibroids may take more time than a simple diagnostic hysteroscopy.
Patient’s Anatomy:
The anatomy of the patient’s uterus can also influence the duration of the works. In some cases, the hysteroscope may need to navigate carefully to access certain areas, which may add to the procedure time.
Experience of the Healthcare Provider:
How long does a Hysteroscopy take, the experience and skill of the healthcare provider performing the process can impact the efficiency of the procedure.
Use of Anesthesia:
Whether the process is performed under local anesthesia or general anesthesia can also affect the overall procedure time.
Additional Procedures:
How long does a Hysteroscopy take, sometimes a process may be combined with other procedures such as endometrial biopsy or insertion of an intrauterine device which can add to the total procedure time.
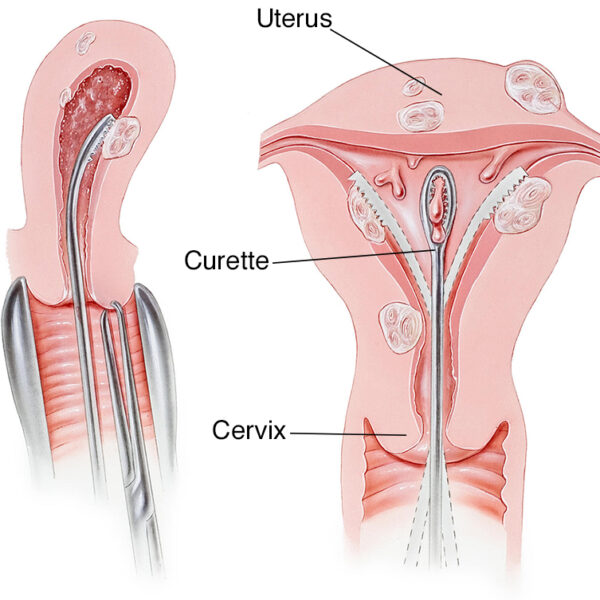
When is Hysteroscopy done – How long does a Hysteroscopy take
Hysteroscopy is performed for both diagnostic and operative purposes. How long does a Hysteroscopy take, it can be scheduled at different times depending on the specific reasons for the procedure.
Diagnostic Hysteroscopy:
- Abnormal uterine bleeding: When a woman experiences heavy, prolonged, or irregular menstrual bleeding.
- Unexplained infertility: To assess the uterine cavity for abnormalities that might hinder implantation or pregnancy.
- Recurrent miscarriages: To check for uterine abnormalities or other factors that might contribute to pregnancy loss.
- Uterine polyps or fibroids: To identify and evaluate the size and location of these growths within the uterus.
- Adhesions: To diagnose and assess scar tissue or adhesions inside the uterus.
- Abnormal findings on imaging tests. For example: ultrasound or Hysterosalpingograph.
Operative Hysteroscopy:
- Treatment of uterine adhesions or scar tissue to improve the uterine cavity’s condition.
- Correction of certain congenital uterine abnormalities (e.g., uterine septum).
- Endometrial ablation to reduce heavy menstrual bleeding.
- Placement of intrauterine devices (IUDs) for contraception or other medical purposes.
- Removal of uterine polyps or fibroids that are causing symptoms or affecting fertility.
Potential Risks and complications
Bleeding:
Some patients may experience light bleeding after the procedure, which usually subsides quickly. In rare cases, there may be more significant bleeding that requires medical attention.
Infection:
There is a small risk of infection following hysteroscopy, especially if the instruments used are not properly sterilized.
Perforation:
In rare cases, the hysteroscopy can accidentally perforate the uterus or nearby organs. This risk is higher during operative hysteroscopy when surgical instruments are used.
Reaction to anesthesia:
If anesthesia or sedation is used during the procedure, there is a small risk of adverse reactions.
Fluid overload:
If a large amount of fluid is used to expand the uterus during the procedure, there is a slight risk of fluid overload especially in patients with certain medical conditions like heart or kidney problems.
Allergic reactions:
Some patients may have allergic reactions to medications or substances used during the procedure.
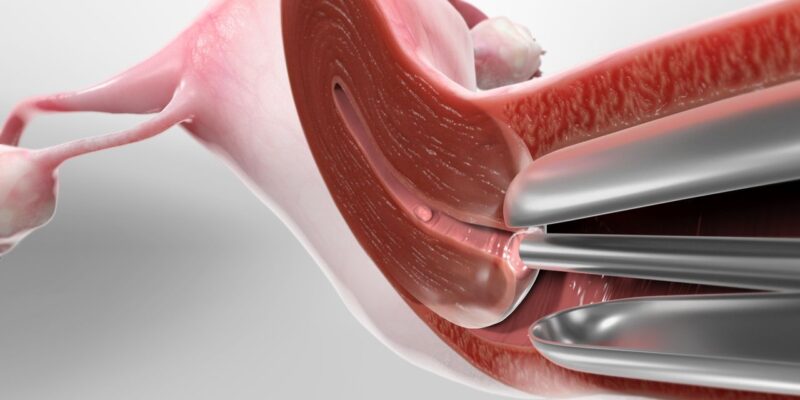
Hysteroscopy under general anesthesia
Complete Comfort:
The patient is completely asleep and will not feel any pain or discomfort during the hysteroscopy.
Muscle Relaxation:
General anesthesia induces muscle relaxation, which can make it easier for the hysteroscope to be inserted into the uterus.
Optimal Conditions:
Since the patient is not moving or feeling pain, the surgeon can focus on performing the procedure more effectively and efficiently.
What happens during a hysteroscopy?
Diagnostic Hysteroscopy:
- Before the procedure:
How long does a Hysteroscopy take, the patient may be given anesthesia or a sedative to help relax and reduce discomfort.
- Insertion of the hysteroscope:
A hysteroscope is a thin, lighted tube with a camera attached to it. It is inserted into the vagina, through the cervix, and then gently moved into the uterus. The camera allows the doctor to view the uterine cavity on a monitor.
- Filling the uterus:
A sterile fluid is pumped into the uterus through the hysteroscope to expand the uterine cavity and allow better visualization.
- Examination:
The doctor examines the uterine lining, looking for abnormalities, such as polyps, fibroids, adhesions. Other issues that may be causing symptoms like abnormal bleeding or infertility.
- Biopsy:
If any abnormal tissue is found, the doctor may take a small sample for further testing in a laboratory.
Operative Hysteroscopy:
- Surgical instruments:
To perform procedures like removing polyps or fibroids, excising adhesions, or placing contraceptive devices like intrauterine devices (IUDs).
- Electrosurgery or laser:
In some cases, electrosurgical or laser techniques may be used to treat abnormal tissue by cutting or coagulating it.


1 Comment